Diabetes is a chronic condition where the body struggles to process sugar. You have type 1 diabetes, where your body doesn’t produce insulin, and type 2, which often stems from lifestyle. Recognizing early symptoms can make a big difference in managing and even preventing complications.
Men and women might share some common symptoms, but there are a few that men should particularly watch out for. Knowing these can lead to quicker diagnosis and better treatment outcomes. And hey, early action can help you avoid some serious health issues down the line.
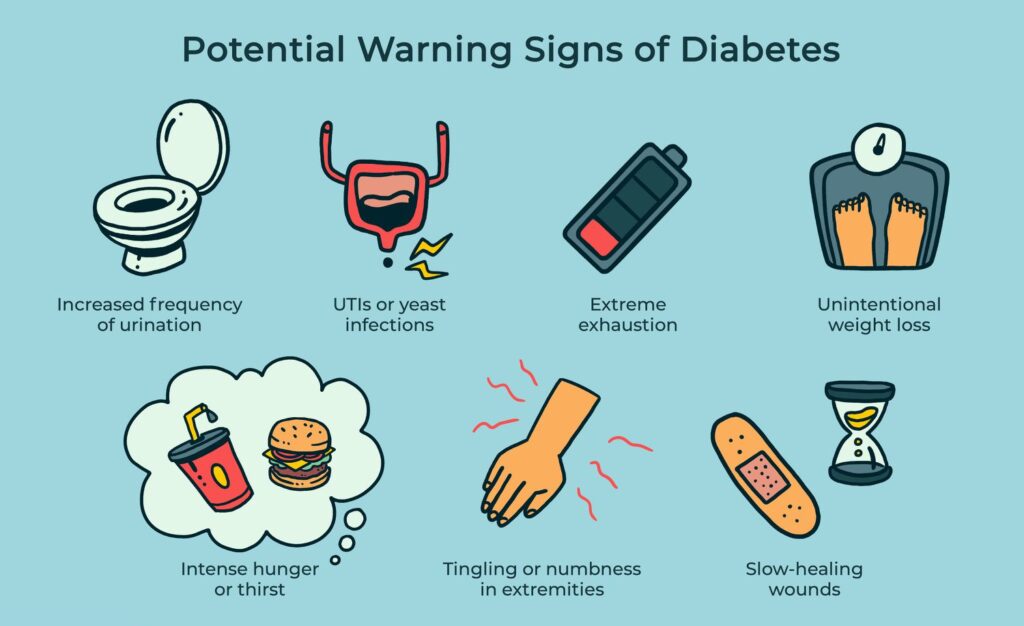
It’s not all gloom and doom, though. With the right knowledge and habits, you can manage diabetes effectively. This article will guide you through the early warning signs to keep an eye on, and provide practical tips to make life easier if you notice any of these signals.
Frequent Urination: A Key Early Indicator
Frequent urination is something you definitely want to pay attention to. When you’re heading to the bathroom more often than usual, it might be because your kidneys are working overtime to eliminate excess sugar from your bloodstream. This can be one of the first red flags that something’s off.
It might seem like a minor inconvenience at first. But think about how annoying it gets when you’re constantly interrupted by the urge to go. It’s not just about drinking too much water or caffeine. If you’re finding yourself up multiple times a night, it’s worth a closer look.

So what’s the deal here? High blood sugar levels cause your kidneys to pull extra water from your blood to help flush out that sugar. This leads to more frequent trips to the bathroom, both day and night.
Managing frequent urination can make a big difference in your daily life. Cut back on sugary drinks, even those that seem healthy, and keep an eye on your overall fluid intake. Staying hydrated is important, but you’ll want to pace yourself with water throughout the day rather than chugging a lot at once.
If you’re noticing this symptom, it’s a good idea to keep a log of how often it happens and mention it to your doctor. They can run some tests and help figure out what’s going on. The sooner you catch it, the better your chances of managing it effectively.
Dry Mouth and Excessive Thirst
Experiencing a parched mouth can be more than just annoying—it might be your body’s way of telling you that something is up, especially when it comes with an insatiable thirst. Just like frequent urination, these symptoms are tied to how your body handles sugar.
When your sugar levels are high, it pulls fluids from your tissues, leaving you with that constant dry mouth feeling and driving you to drink more. No matter how much water you gulp down, it often feels like you can’t quench your thirst.

Staying hydrated is crucial, but pay attention if you find yourself constantly reaching for your water bottle. Opt for water over sugary or caffeinated drinks, which can make things worse. Try eating hydrating foods like cucumbers and watermelons, and keep track of your fluid intake.
Dry mouth can also wreak havoc on your oral health. Without enough saliva, bacteria can thrive, leading to bad breath, gum disease, and cavities. Make sure you’re brushing twice a day, flossing, and maybe even rinsing with a mouthwash that’s gentle on your gums.
If excessive thirst and dry mouth are causing real discomfort, your best move is to talk to your doctor. They can help pinpoint the cause and suggest ways to keep your hydration and health in good balance. Catching these signs early can help you prevent more significant issues down the road.
Dry Skin: A Common but Overlooked Symptom
Dealing with dry skin is part of the package for many with diabetes. You might notice your skin feeling tight, itchy, or even cracking. This is particularly true in areas like your elbows, feet, and legs.
High blood sugar levels can affect your skin’s health, making it more prone to drying out. When your body is dehydrated—or if you’re losing fluids quickly—it can leave your skin lacking moisture. Add that to potential circulation issues in diabetics, and your skin takes a hit.
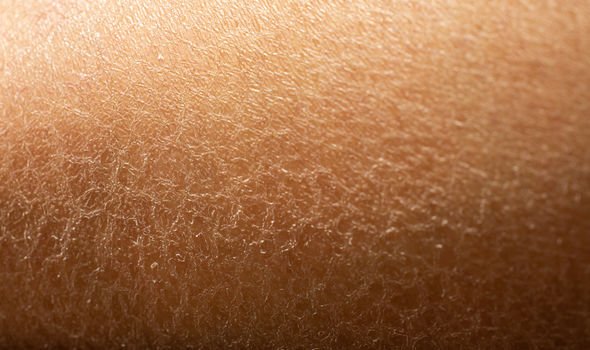
Combatting dry skin starts with a good moisturizer. Go for lotions that are fragrance-free and designed for sensitive skin. Apply it right after you shower, and keep some handy to reapply throughout the day, especially in colder weather.
Stay vigilant about your skin’s condition. Keep an eye out for cracks or sores that just won’t heal. Dry skin can lead to infections, which are more challenging for diabetics to fend off. Simple habits like wearing sunscreen, drinking plenty of water, and using a humidifier can make a difference.
If things don’t seem to improve, it might be time to visit a dermatologist. They can help tailor a skincare routine that addresses your specific needs and keeps your skin in good shape, despite diabetes.
Slow-Healing Wounds and Infections
Slow-healing wounds are a significant concern for those with diabetes. If you notice cuts or sores that linger far longer than usual, your body could be signaling an issue with high blood sugar levels. When sugar levels are high, your immune system doesn’t function as effectively, which means minor injuries can become big problems.
Men often overlook small cuts or abrasions, but with diabetes, it’s crucial to give them proper attention. Bacteria thrive in high-sugar environments, and slow healing can make it easier for infections to set in. This can lead to serious complications like ulcers or even the dreaded hospital visits.
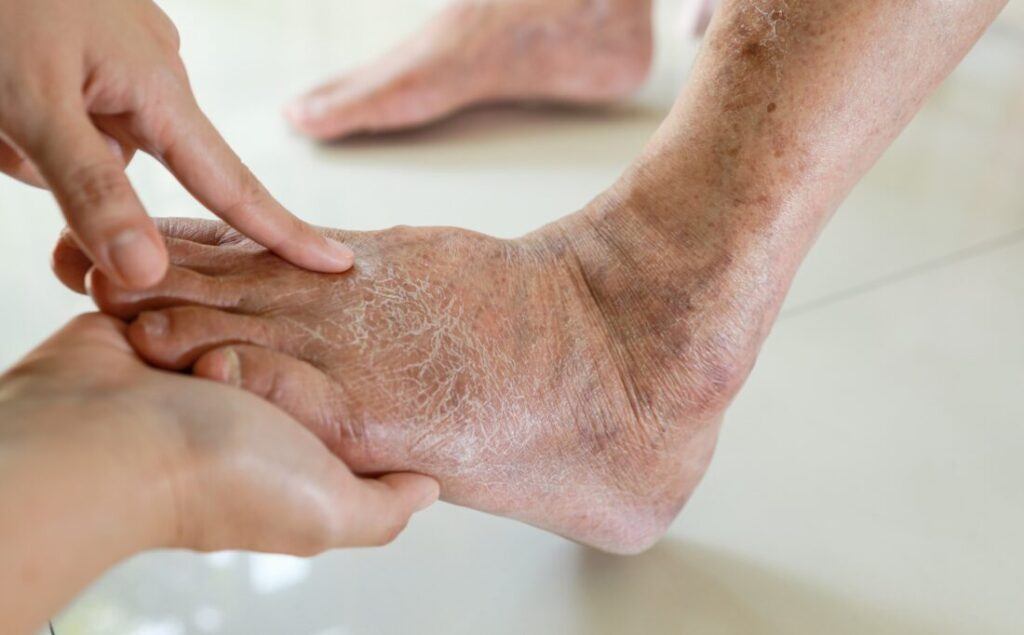
To minimize these risks, make a habit of checking your skin daily for any cuts, blisters, or sores, especially on your feet. Clean any wounds promptly and apply antibiotic ointment to help keep infections at bay. It’s a good idea to keep your toenails trimmed and wear comfortable shoes that don’t cause friction.
A crucial prevention tactic involves managing your blood sugar levels. Keeping them within the recommended range not only helps with overall health but also boosts your body’s ability to heal. Regular exercise, a balanced diet, and medication as prescribed are key elements in controlling sugar levels.
If a wound doesn’t show signs of healing within a reasonable time or appears to be getting worse, consult a healthcare professional. Early intervention can prevent complications and ensure that your wounds heal correctly.
Vision Problems: Blurry Vision and Eye Difficulties
Blurry vision can be one of the early warnings of diabetes. If you notice things looking fuzzier than usual, it might be more than just needing new glasses. High blood sugar levels can cause your eye lenses to swell, making it harder to focus.
Ignoring blurred vision can lead to more severe conditions like diabetic retinopathy, where blood vessels in the eye get damaged. Over time, this can lead to vision loss if not treated promptly.

To protect your vision, keep a close watch on your blood sugar levels, as consistent management can prevent these eye changes. Regular eye exams are essential. Make sure your eye doctor knows about your diabetes so they can check for specific issues, like changes in your retina.
Wearing polarized sunglasses can reduce glare and help you see better outdoors. Also, using artificial tears can alleviate dry eyes, which can be more common when you have diabetes.
If you experience sudden changes in vision, such as seeing floaters or flashes of light, seek medical advice right away. Prompt treatment can make a significant difference in preserving your eyesight.
Unexpected Weight Loss
Shedding pounds without trying might sound like a dream, but it’s often a worrying sign when it comes to diabetes. When your body can’t use glucose for energy due to a lack of insulin, it starts burning fat and muscle instead. This can lead to rapid, unintentional weight loss.
Spotting early weight loss is crucial. If you’ve dropped a significant amount without changing your diet or exercise routine, take notice. Track your weight and discuss any unexplained changes with your doctor.
 Distinguishing between healthy and unhealthy weight loss is important. While a balanced diet and exercise can help manage diabetes and promote weight loss, rapidly losing weight without these changes can signal a problem.
Distinguishing between healthy and unhealthy weight loss is important. While a balanced diet and exercise can help manage diabetes and promote weight loss, rapidly losing weight without these changes can signal a problem.
Adjusting your diet can help stabilize weight. Incorporate more proteins and healthy fats, which provide sustained energy and help maintain muscle mass. Cruciferous vegetables like broccoli and cauliflower are excellent additions due to their low carb content and high fiber, keeping you full without spiking blood sugar.
Consulting a nutritionist can be a game-changer. They can tailor a meal plan to your needs, ensuring you’re getting the right nutrients while managing your blood sugar levels. Combining dietary changes with regular exercise can help maintain a healthy weight.
Healthy Lifestyle Tips and Nutritional Guidance
Managing diabetes isn’t just about keeping an eye on early signs; it’s also about making lasting lifestyle changes that keep you healthy. Diet and exercise play vital roles in controlling blood sugar levels and overall well-being.
Starting with your diet, prioritize whole foods over processed ones. Cruciferous vegetables are a fantastic choice as they are low in carbs but high in nutrients. Think broccoli, cauliflower, and Brussels sprouts—they’re not only filling but also help regulate blood sugar.
Protein is key, too. Lean meats, fish, eggs, and plant-based proteins like beans and lentils can help stabilize your energy levels. Spread your protein intake throughout the day to maintain steady blood sugar levels. Avoid high-sugar snacks and opt for nuts or a piece of fruit instead.
Regular exercise can’t be overstated. Aim for at least 30 minutes of moderate activity most days of the week. This could be anything from walking and jogging to swimming or cycling. Exercise helps your muscles use glucose more effectively, lowering your blood sugar in the process.

Stay on top of your condition by regularly monitoring your blood sugar levels. This will help you understand how different foods and activities impact your glucose. Learn how to adjust your diet and exercise based on these readings.
Consistency is your best friend here. Small, manageable changes are easier to stick with and can make a big difference over time. Partner with a healthcare provider to create a plan that’s customized for you.
Lastly, don’t underestimate the power of support. Whether it’s family, friends, or support groups, having people who understand what you’re going through can provide emotional and practical assistance.





